Brain Problems Linked to Even Mild Coronavirus Infections, UK Study Finds
Team finds acute disseminated encephalomyelitis diagnoses not linked to severity of COVID-19; survey carried out on 43 patients hospitalized in confirmed or suspected virus cases.
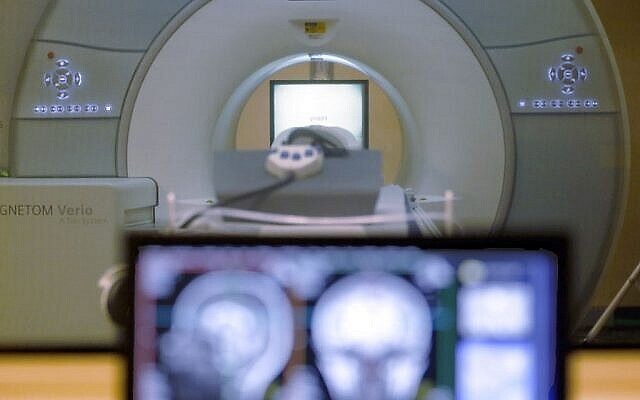
Potentially fatal COVID-19 complications in the brain including delirium, nerve damage and stroke may be more common than initially thought, a team of British-based doctors warned Wednesday.
Severe COVID-19 infections are known to put patients at risk of neurological complications, but research led by University College London suggests serious problems can occur even in individuals with mild cases of the virus.
They found 10 cases of temporary brain dysfunction, 12 cases of brain inflammation, eight strokes and eight cases of nerve damage.
Most of those patients with inflammation were diagnosed with acute disseminated encephalomyelitis (ADEM) — a rare condition typically seen in children after viral infections.

“We identified a higher than expected number of people with neurological conditions such as brain inflammation, which did not always correlate with the severity of respiratory symptoms,” said Michael Zandi, of UCL’s Queen Square Institute of Neurology and University College London Hospitals NHS Foundation Trust.
The research, published in the journal Brain, showed that none of patients diagnosed with neurological problems had COVID-19 in their cerebrospinal fluid, suggesting that the virus did not directly attack their brains.
Perhaps crucially, the team found that ADEM diagnoses “not related to the severity of the respiratory COVID-19 disease.”
“Doctors need to be aware of possible neurological effects, as early diagnosis can improve patient outcomes.”
With more than 11 million confirmed infections worldwide, COVID-19 is known to cause a variety of health complications in addition to lung infection.
While the results of the study suggest that brain complications could be more common among virus patients than first thought, experts said it didn’t mean that brain damage cases were widespread.
“The scrutiny that the pandemic attracts means it would be very unlikely that there is a large parallel pandemic of unusual brain damage linked to COVID-19,” said Anthony David, director of UCL’s Institute of Mental Health.






comments